Cervicogenic Headache
Overview
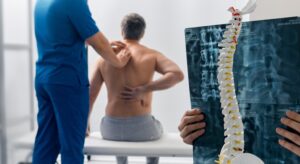
A cervicogenic headache is a type of headache that originates from the neck. The pain is caused by problems in the cervical spine, including joints, muscles, or nerves, but is felt in the head.
Because the nerves in the upper neck share pathways with nerves in the head, pain from the neck can be perceived as a headache. This condition is often mistaken for migraines or tension headaches.
Symptoms
Cervicogenic headaches typically have distinct features:
- One-sided head pain
- Pain that starts in the neck and spreads to the head
- Headache triggered by neck movement or certain positions
- Reduced range of motion in the neck
- Tenderness at the base of the skull
Less common symptoms may include mild sensitivity to light or sound, but these are usually not as prominent as in migraines.
Causes
Cervicogenic headaches are caused by issues affecting the neck.
Common causes include:
- Degeneration of cervical joints and discs
- Injury to the neck, such as whiplash
- Poor posture or repetitive strain
- Inflammation or dysfunction of upper cervical joints
Any condition that affects the upper cervical spine can lead to this type of headache.
Diagnosis
Diagnosis begins with a medical history and physical examination. A doctor will assess neck movement, pain patterns, and areas of tenderness.
Imaging tests may be used to evaluate the cervical spine, including:
- X-rays to assess alignment and joint changes
- MRI scans to evaluate soft tissues and nerves
- CT scans for detailed images of bone structures
In some cases, diagnostic nerve blocks may be used to confirm the source of pain.
Treatment Options
Treatment focuses on relieving pain and addressing the underlying neck issue.
Common treatment options include:
- Pain medications, including NSAIDs
- Muscle relaxants or other prescription medications
- Physical therapy to improve strength, mobility, and posture
- TENS (transcutaneous electrical nerve stimulation)
If symptoms persist, additional treatments may include:
- Nerve blocks to reduce inflammation and confirm the pain source
- Radiofrequency ablation to block pain signals
Surgery is rarely needed but may be considered in severe cases when other treatments do not provide relief.